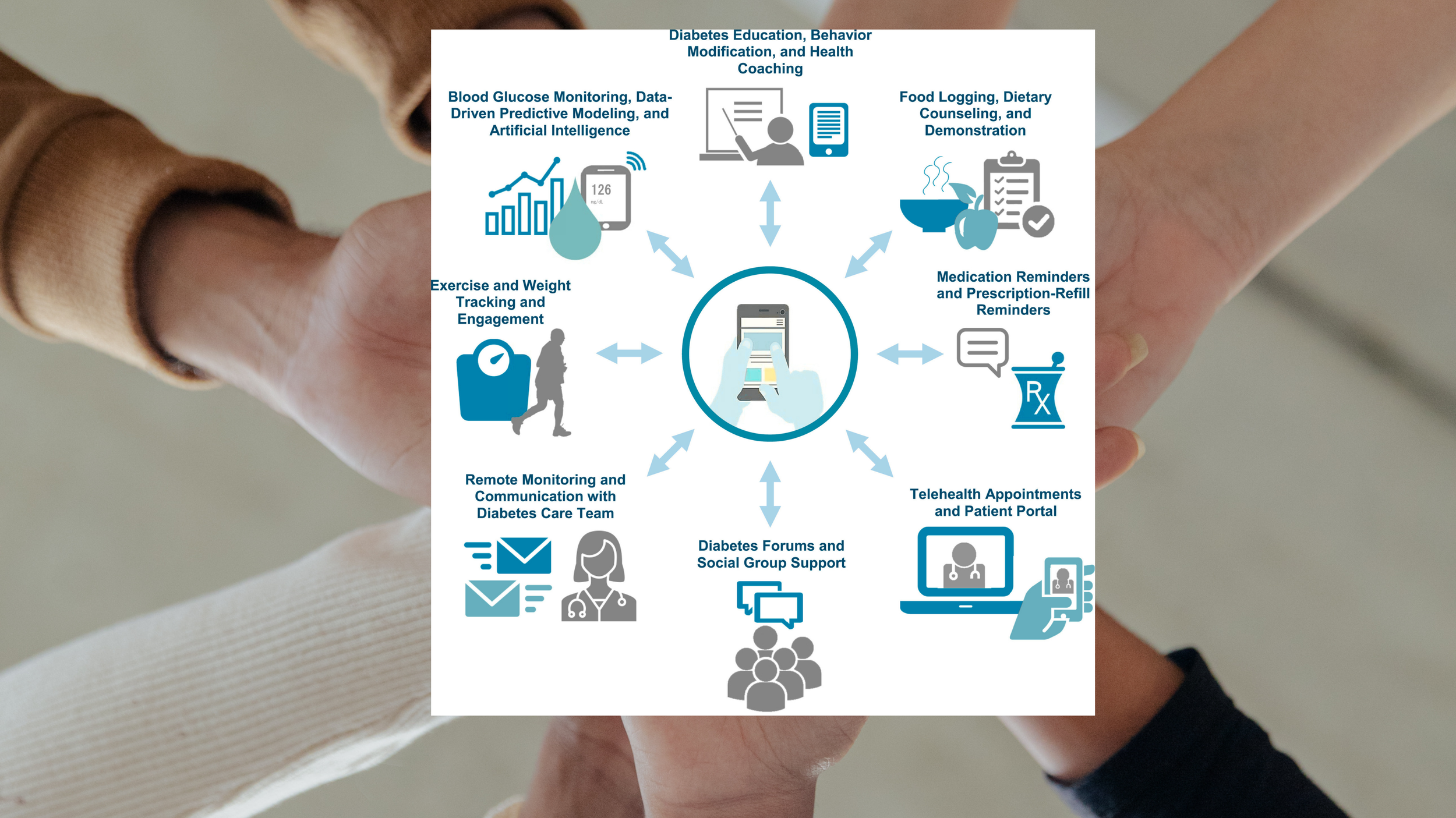
Core Service Packages
Culturally tailored diabetes education
African diabetes nutrition
Diabetes education for Africans and diaspora
Virtual diabetes coaching
Key Takeaways from the 2026 ADA Standards of Care 🩺📘
The 2026 Standards of Care from the American Diabetes Association highlight a continued shift toward earlier screening, individualized treatment, expanded use of technology, and equity-focused diabetes management.
These updates are designed to improve outcomes while addressing real-world barriers to care—especially for underserved populations.
Below are the key highlights clinicians, educators, and patients should know.
🔍 Screening & Diagnosis
Earlier screening
Routine diabetes screening now begins at age 35 for all adults, with earlier screening recommended for those with additional risk factors.
Youth screening
Children and adolescents with overweight or obesity and risk factors should be screened for prediabetes and type 2 diabetes.
Neonatal diabetes
Genetic testing is recommended for diabetes diagnosed before 6 months of age, with sulfonylurea therapy for KATP-related cases.
📊 Glycemic Monitoring
Expanded CGM use
Continuous glucose monitoring (CGM) is recommended at diagnosis and ongoing for adults using insulin or at high risk for hypoglycemia, with consideration for basal insulin users.
Beyond A1C
The guidelines recognize limitations of A1C testing. CGM metrics or fructosamine should be used when A1C results are unreliable.
Individualized targets
Glycemic goals should be tailored based on comorbidities, life expectancy, and hypoglycemia risk, with de-intensification when benefits are limited.
💊 Pharmacologic Therapy
Cardiorenal protection first
SGLT2 inhibitors and GLP-1 receptor agonists are prioritized for patients with cardiovascular disease, heart failure, or chronic kidney disease—regardless of A1C level or metformin use.
Early combination therapy
Combination therapy may be initiated at diagnosis for individuals with A1C >8.5% or high cardiorenal risk.
Insulin initiation
When insulin is started, it should be combined with diabetes self-management education and support (DSMES), while continuing metformin and cardiorenal-protective agents when appropriate.
🧠 Lifestyle & Diabetes Education
DSMES is essential
Diabetes self-management education and support is recommended at diagnosis, annually, and whenever health status or treatment changes.
Weight management
A 5–15% weight loss is targeted for metabolic improvement and potential diabetes remission.
Physical activity
Exercise recommendations should be individualized, with appropriate screening for diabetes-related complications.
❤️ Cardiovascular & Renal Risk Management
Blood pressure targets
For high-risk patients, blood pressure targets are now <120 mmHg, when safe and individualized.
Statin therapy
Statins are recommended for primary prevention in adults aged 40–75 years with diabetes.
Chronic kidney disease care
SGLT2 inhibitors or GLP-1 receptor agonists are recommended to slow CKD progression and reduce cardiovascular events.
🌍 Equity & Special Populations
Older adults
CGM is encouraged for insulin-treated older adults, with blood pressure goals tailored to overall health status.
Social determinants of health
Assessment and intervention addressing social determinants of health are essential to reducing disparities in diabetes outcomes.
Advocacy priorities
The guidelines emphasize insulin affordability, employment protections, and equitable access to care across all settings.
🤝 Implementation & Quality Improvement
Team-based care
Coordinated, interdisciplinary care is essential for effective diabetes management.
Technology access
Technology adoption should expand while actively addressing cost and access barriers.
Education and training
Ongoing workforce development and evidence-based practice remain central to high-quality care.
Bottom Line
The ADA 2026 Standards of Care prioritize early detection, personalized treatment, cardiorenal protection, expanded diabetes technology, and health equity—all aimed at improving outcomes and reducing disparities.
At Vieve Health & Wellness, these principles guide how we educate, coach, and support individuals living with or at risk for diabetes—especially within African and diaspora communities.
💬 How are you integrating these updates into your clinical practice or diabetes education efforts?
—
Dr. Genevieve Ufongene, DNP, FNP-C
Founder, Vieve Health & Wellness
#ADA2026 #DiabetesCare #CGM #CardiorenalHealth #DSME #HealthEquity #EvidenceBasedCare #DiabetesEducation
Education Without Overwhelm
Who it’s for:
Newly diagnosed with diabetes or prediabetes
Africans & diaspora confused about food and blood sugar
People who want clarity before committing long-term
What’s included:
60-minute 1:1 virtual diabetes education session
Understanding diabetes in simple, practical terms
How African foods affect blood sugar
Portion guidance using familiar meals
Blood sugar basics (what numbers mean & patterns)
Personalized education summary (PDF)
7-day email/WhatsApp follow-up
Client outcome:
“I finally understand my diabetes.”
Who it’s for:
People who know what to do but struggle to stay consistent
Clients tired of trial-and-error dieting
Those who want support, not lectures
What’s included:
4 weekly 45-minute 1:1 coaching sessions
Personalized food strategies using cultural foods
Lifestyle coaching (sleep, stress, movement)
Blood sugar log review & feedback
Weekly action steps
Educational handouts
Support between sessions (WhatsApp/email)
Client outcome:
“I feel confident, supported, and in control.”
👉 CTA: Start Coaching with Me

2025
New York
The Atlast Project →
“Communication was top-notch and the final outcome was even better than we imagined. A great experience all around.”
Former CustomerGet In Touch
If you're interested in working with us, complete the form with a few details about your project. We'll review your message and get back to you within 48 hours.